Having a new baby is scary business for most new parents. There are so many transitions and things baby goes through, it is hard to tell what’s normal and what’s not. Here are a few of the most common problems you may experience with your newborn.
Jaundice
Jaundice is the yellowing of baby’s skin....
Know before you go: medical terms you might hear during labor and delivery
Even if you attend childbirth classes and read extensively about childbirth, some terms that the doctors and nurses use during labor may be unfamiliar to you. Let’s walk through some common childbirth terms that you might hear once you get to Huntsville Hospital for Women & Children or Madison...
Let’s get serious for a minute
Let’s talk about a serious but not uncommon health issue affecting many pregnant mothers: substance abuse.
First, remember that you are not alone. Substance abuse can be the abuse or misuse of legal and illegal substances, but many of these substances can cause health concerns for mom and baby because...
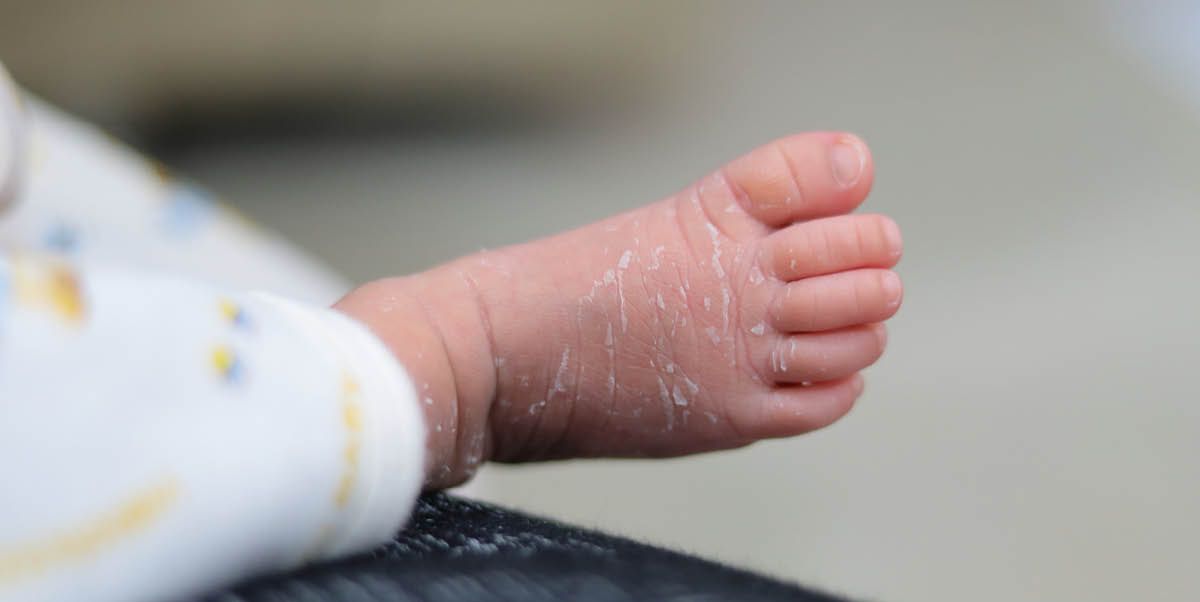
For baby’s health, just say cheese
Let’s talk about baby’s skin and that cheesy white substance they are born with. What is it, and how does it benefit your baby?
The scientific name of that cheesy white substance is vernix caseosa – vernix, for short. Vernix is a coating on baby’s skin made up of fatty secretions and dead skin cells,...
How to choose the right car seat before you hit the road with baby
Now that your precious baby has arrived, it’s time to focus on keeping her safe – at home and in the car.
Did you know car crashes are the leading cause of death for children between 1 and 13 years old? At Huntsville Hospital for Women & Children and Madison Hospital, we want car seat safety to...
Sorting out breastfeeding facts from fiction
When it comes to women’s health, there’s so much information online that it can be hard to tell fact from fiction. We asked two of our breastfeeding experts – International Board Certified Lactation Consultants Erica Elkins and Jessie Jankens – to address some common myths about breastfeeding.
Myth:...
Your baby has arrived. Now what?
Once baby arrives you will transition into the fourth trimester, also known as postpartum.
You can expect to undergo physical as well as emotional changes over the next few weeks as you return to your normal, pre-pregnancy state. During this time, it is important to keep a watchful eye on vaginal...
Why breastfeed? Let’s talk about the benefits
What do I need to know to be successful at breastfeeding my baby?
Many new mothers ask themselves this question at some point during their pregnancy and journey into parenthood. The benefits of breast milk to nourish and protect your baby’s immature immune system are well established, but did...
Not eating well because of morning sickness? You may need a prenatal vitamin
Did you know that pregnancy increases your needs for 20 out of 29 necessary vitamins and minerals, and that your B6, folic acid, iron, iodine and zinc needs are increased 40-50 percent?
At any life stage, eating a variety of proteins, whole grains, fruits, vegetables, and calcium-rich foods can meet...
What to do if you experience postpartum hemorrhage
Postpartum hemorrhage (PPH) is a serious but rare condition when a woman has heavy bleeding after giving birth. You’re more likely to have PPH if you’ve had it in the past or if you have certain medical conditions – especially conditions that affect the uterus (womb) or the placenta or conditions...